
Maimonides Summer Research Experience
Founded by Dr. Afshin Razi, Dr. Jack Choueka and Dr. Rushabh Vakharia in 2020, the Maimonides Summer Research Experience invites ten first-year medical students to participate in an eight-week research program.
World-class bone and joint care here in your neighborhood.








Maimonides Bone & Joint Center is the only orthopedic center in NYC to earn Healthgrades’ Orthopedic Surgery Excellence Award in 2023 and has received Five-Stars for Hip Fracture Treatment for 4 years in a row. With six convenient locations, we offer comprehensive orthopedic, sports medicine, orthopedic oncology, treatment of the upper and lower extremities, joint replacement, and trauma services.
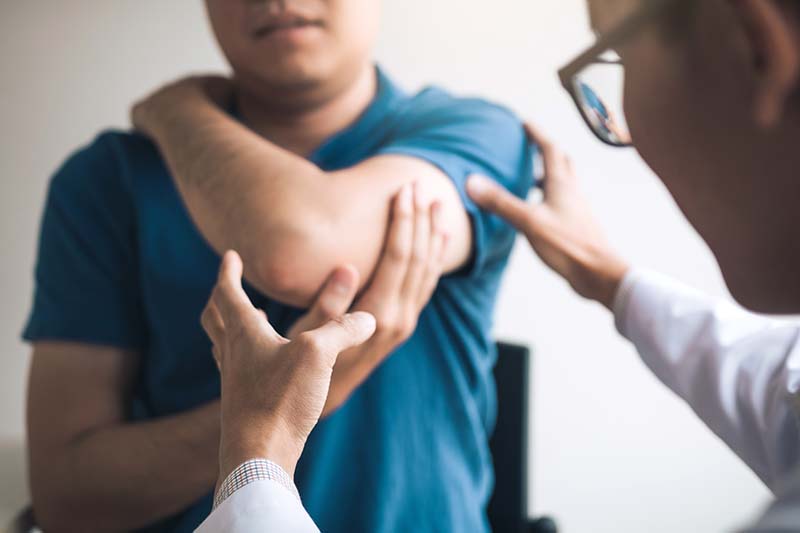
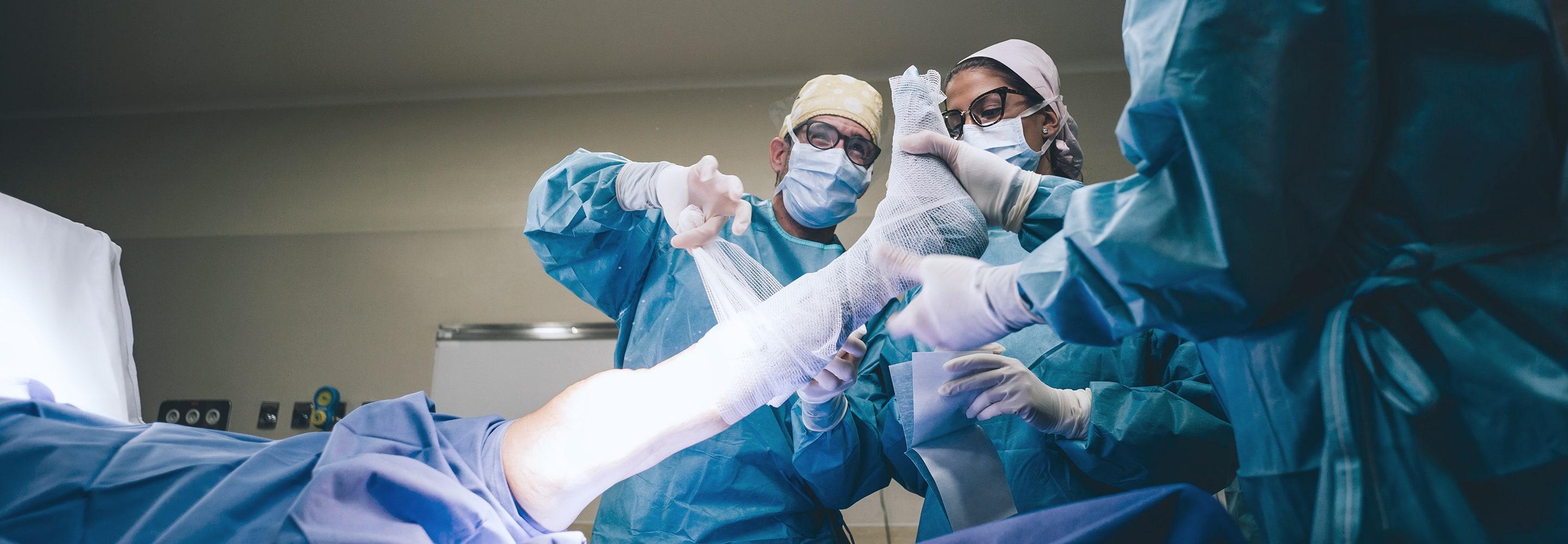
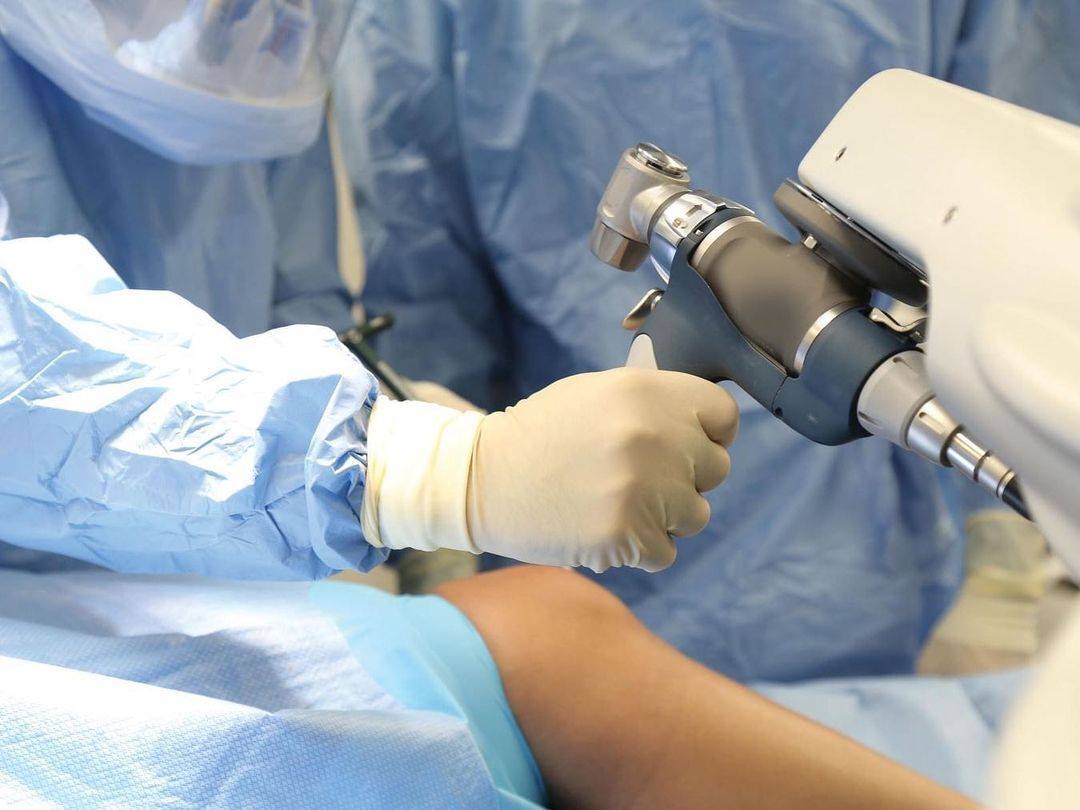
If you need a knee or hip replacement, Maimonides Bone & Joint Center is proud to be the first hospital in Brooklyn to perform joint replacement surgery using a robotic arm-assisted system. This pioneering minimally-invasive technology means even more precise surgeries and better outcomes for patients.

Founded by Dr. Afshin Razi, Dr. Jack Choueka and Dr. Rushabh Vakharia in 2020, the Maimonides Summer Research Experience invites ten first-year medical students to participate in an eight-week research program.

Childbirth can be an exciting, joy-filled experience. But for millions of pregnant patients every year, labor and delivery presents potentially dangerous health complications. Catching the
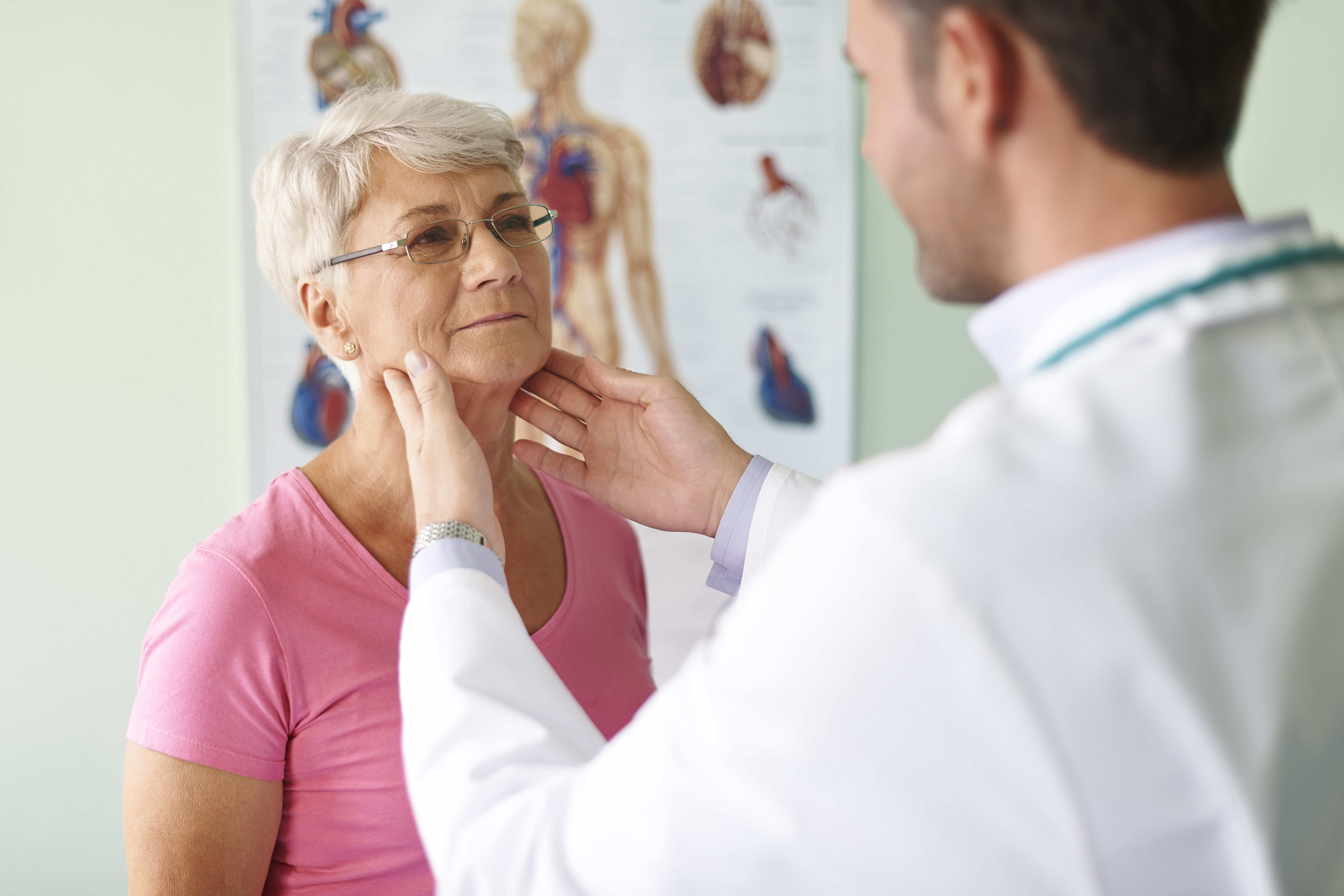
Helping patients who have undergone a total laryngectomy recover their speaking ability is critical to their return to normalcy and maintaining a high quality of
